 
Simply put, it has a low chance of appeal after you’ve received the denial, thus you lose money. Submitting a claim past an insurance's timely filing limit will come back to you as Claim Adjustment Reason Code (CARC) 29 and state, “The time limit for filing has expired.”ĬARC 29 has a high chance of prevention but a low overturn rate. On the flipside, if your team isn't familiar with the limits for the insurances the majority of your patients use, you're losing revenue. 
Knowing the deadlines of payers that attribute to most of your revenue before your patients visit your office will help your team anticipate and submit your claims faster. 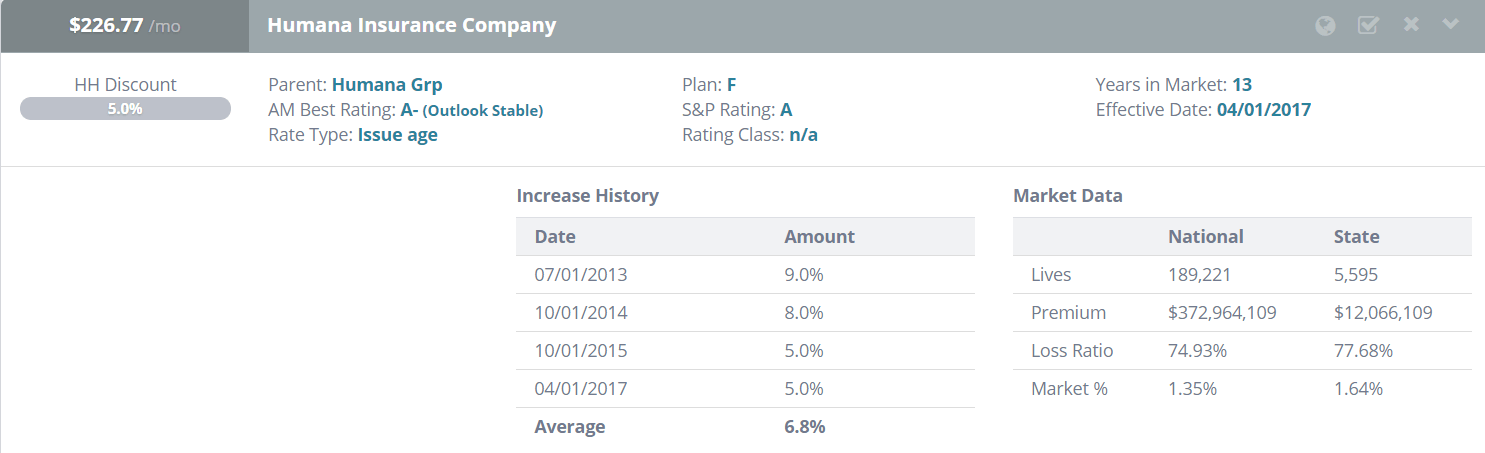
Why not use it as a guide to help identify the most important timely filing limits your team should be aware of? It's helpful in breaking down what percentage of revenue comes from common insurances. When speaking to our clients, most of them know their payer mix.Ī payer mix is a listing of the different healthcare insurances your patients use. But which are they actually using? Of course, I'm referring to what's known within the industry as a "payer mix." There are hundreds of thousands of insurance options your patients can choose from. Some of those responsibilities include patient care, coding, and keeping track of healthcare requirements.Įnsuring your team is submitting patient claims on time is another important responsibility you need to know. With a small amount of extra effort, you can lower your timely filing denial rate even more.Ĭhances are, you and your staff already have a ton of work to complete on a daily basis. As a simple example for reference, 0.01% of $3,000,000 is $30,000.įurthermore, that percentage is only true if you have all of those payers and submit an equal amount of claims to each. If the deadline isn’t 180 or 365 days then there’s a 56% chance that the limit is 90 daysīy submitting your claims within 90 days the chances that you receive a claim denial related to timely filing is 0.01%.Ī 0.01% chance stacks the odds in your favor, although that percentage can still have a significant negative effect on your bottom line if you aren't vigilant. If the deadline isn’t 180 days then there is a 46% chance that their limit is 365 days There is a 34% chance that an insurance company has a deadline of 180 days The two most popular timeframes are 180 days and 360 days If the plan decides against you (fully or partially), your appeal is automatically sent to level 2.From the bar graph and statistical data above we can conclude that… Your plan will tell you the reasons for the delay and inform you of your right to file an expedited (fast) grievance if you disagree with the plan’s decision to take an extension. Your plan will notify you in writing if it decided to take an extension. For example, if your plan needs more information from a non-contract provider to make a decision about the case, and the extension is in your best interest. The time to complete standard and fast service requests may be extended by up to 14 days in some cases. You'll get a fast request if your plan determines, or your doctor tells your plan, that waiting for a standard service decision may seriously jeopardize your: How long your plan has to respond to your request depends on the type of request: Keep a copy of everything you send to your plan as part of your appeal. Include any other information that may help your case. 
If you've appointed a representative, include the name of your representative and proof of representation.47 Electronic funds transfer (EFT/Electronic. The items or services for which you're requesting a reconsideration, the dates of service, and the reason(s) why you're appealing. Humana Healthy Horizons® in Louisiana is a Medicaid product of Humana Health Benefit Plan of Louisiana Inc.Your name, address, and the Medicare number on your Medicare card.Include this information in your written reconsideration request: You, your representative, or your doctor must file a written standard or expedited (fast) request, unless your plan allows you to file a request by phone, fax, or email. If your appeal is for a service you haven’t gotten yet, your doctor can ask for a reconsideration on your behalf and must notify you about it. You must ask for a reconsideration within 60 days of the date of the organization determination. If you disagree with the initial decision from your plan (also known as the organization determination), you or your representative can ask for a reconsideration (a second look or review). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
